
Pancreatic Cancer Treatment Options That Can Extend Lives
The AdventHealth Digestive Health Institute’s surgeons are committed to treating pancreatic cancer, working to provide patients with better treatment options and improve survival rates. The pancreas is a large organ located behind the stomach that functions as both a digestive and hormonal gland. During digestion, it produces and releases enzymes that assist the body in absorbing foods and especially fats. The pancreas also makes insulin and glucagon, hormones that help the body regulate its blood sugar levels.
Pancreatic cancer occurs when cells in the pancreas develop genetic mutations. These mutations cause the cells to grow and divide uncontrollably. People who smoke or who are obese are at an increased risk for pancreatic cancer, but sometimes it is caused by hereditary factors. Medical conditions that put people at a greater chance of developing pancreatic cancer are diabetes, chronic pancreatitis and cirrhosis of the liver. Pancreatic tumors often have a poor prognosis, even when diagnosed early, because cancer of the pancreas tends to spread rapidly.
Whole-Person Care for Pancreatic Cancer
Signs and symptoms of pancreatic cancer usually do not appear until it is quite advanced.
Symptoms of pancreatic cancer are very similar to those of other digestive cancers and conditions, and can include:
- Pain or discomfort in the upper part of the abdomen
- Jaundice, or yellowing of the skin and eyes
- Loss of appetite
- Unintended weight loss
- Dark urine
- Light-colored stools
- Itchiness
- Weakness
- Nausea
Another type of pancreatic cancer, pancreatic neuroendocrine tumor (NET), involves the cells that produce hormones. Symptoms related to a NET involve problems caused throughout the body related to hormone overproduction. These symptoms differ widely depending on the hormone involved but can include acid reflux, diarrhea, high blood sugar, low blood sugar and gallstones.
If your doctor thinks you could have pancreatic cancer or a similar condition, you will likely have:
- Imaging tests to look for tumors in the pancreas and liver. These may include a CT scan, an MRI scan, endoscopic ultrasound (EUS), endoscopic retrograde cholangiopancreatography (ERCP) and others.
- A fine needle aspiration (FNA) may be done through an endoscopic procedure to collect tissue and fluid samples for biopsy.
- A pathologist will study the biopsied cells to determine whether or not they are cancerous.
- In rare cases, biopsy might be skipped. This would be when an imaging test shows the presence of a pancreatic tumor that is very likely to be cancer and able to be completely removed with surgery. If so, surgery will be done to remove the tumor as collecting biopsy samples might cause cancer cells to break off the tumor and spread to other parts of the body.
Surgery is only an option when the cancer is confined to the pancreas. If a pancreatic tumor is able to be completely removed with surgery, patients have a good prognosis. The solution is to remove the affected part of the pancreas, which is called pancreatectomy.
There are two types of pancreatectomies:
- Pancreaticoduodenectomy (Whipple procedure) – For tumors located in the head of the pancreas (or right side)
- Distal pancreatectomy – For tumors in the tail and body of the pancreas (or left side)
To view actual footage of these surgical procedure, please visit the PROCEDURE VIDEOS and ADDITIONAL RESOURCES page in the for medical professionals section of the site.
Minimally Invasive Pancreatectomy and Whipple Procedure
Dr. Ross is highly experienced in performing these procedures with minimally invasive approaches. She is one of the region’s most experienced surgeons in treating pancreatic cancer. Hoping to achieve better outcomes for patients, Dr. Ross has dedicated a large portion of her practice to treating patients with pancreatic cancers and diseases. Additionally, she has served as a lead investigator in clinical trials to discover better ways of offering surgery for pancreatic cancer.
Our surgical team’s experience has taught them that the least invasive ways of performing pancreatectomy are best for patients, so they offer:
- Laparo-endoscopic single site pancreatectomy – The procedure is performed with small instruments through just one small incision made in the patient’s belly button.
- Robotically-assisted pancreatectomy – The procedure is performed with a few small incisions and assisted by the da Vinci® Surgical System.
These minimally invasive procedures are available for patients depending on the type and location of their pancreatic tumors, how close they are to certain blood vessels, and a patient’s body mass index and medical status.
Having a minimally invasive surgery gives patients a faster recovery so they can move on to the next portion of their treatment plans sooner. This is part of the reason why patients with pancreatic cancer experience unusually better outcomes when treated by the surgeons at AdventHealth Digestive Health Institute. Long-term survival rates of patients with pancreatic cancer treated at AdventHealth Digestive Health Institute are two-and-a-half times the national average.
Patients who have surgery for pancreatic cancer will also have chemotherapy and radiation therapy as part of their treatment plans. These options are also available to patients who are unable to have surgery. Chemotherapy uses drugs, taken orally or given by infusion, to kill cancer cells. Radiation therapy uses high-energy X-ray beams to destroy cells and shrink tumors. Your overall treatment plan will be determined by many different factors, including the stage and location of the pancreatic tumor, as well as your age, overall health and personal preferences.
Surgical Cancer Care
-
Esophageal Cancer
Typically esophageal cancer requires surgery in addition to radiation and chemotherapy. Learn more about the surgical treatments our specialists can provide.
-
Gastric/Stomach Cancer
We help diagnose and treat stomach cancer. We even have minimally invasive options. Learn more about how our gastroenterologists can help you.
-
Duodenal/Small Bowel Cancer
Our gastroenterologists diagnose and treat small bowel and duodenal cancer. We offer three minimally invasive treatment options.
-
Pancreatic Cancer
Our surgeons are among the region’s most experienced in pancreatic surgery. We can help treat your cancer with minimally invasive options. Learn more today.
-
Liver Cancer
Our AdventHealth Digestive Health Institute surgeons offer surgical and non-surgical liver cancer treatments, depending on your specific case. Schedule an appointment with one of our gastroenterologists.
-
Gallbladder Cancer
Removing the gallbladder with cancer is a very complex surgery that requires highly experienced surgeons like those at AdventHealth Digestive Health Institute.
-
Colon and Rectal Cancer
Our experienced gastroenterologists can diagnose and treat colon and rectal cancer. Learn more about treatment and surgery options.
-
Anal Cancer
Our colon and rectal surgeons can help diagnose and treat anal cancer. We offer anal cancer surgery when necessary.
-
Public Reporting of Outcomes
Our compassionate medical staff is committed to providing high-quality healthcare services in Hillsborough County.
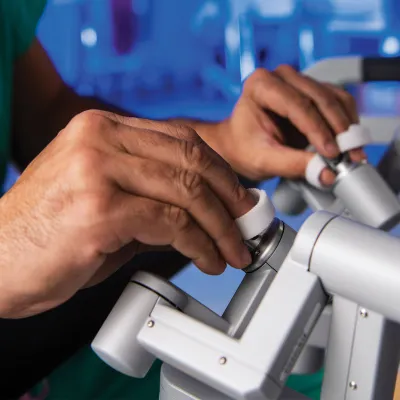
Recover Faster With Minimally Invasive and Robotic Surgery
The expert surgeons at the AdventHealth Digestive Health Institute have a large depth of experience in offering minimally invasive surgery.

Meet Your Dedicated Experts
Our specialists are passionate about providing collaborative care that addresses your unique needs and goals while ensuring you feel informed and supported every step of the way. Learn more about our team and their areas of expertise.

Surgical Consultations For Digestive Cancer Without the Wait
Appointments Within Seven Days for Patients with Cancer
At AdventHealth Digestive Health Institute, we know that after being diagnosed with cancer, patients want and often need to begin treatment quickly. So we make it a priority to offer appointments for cancer surgery consultations within five business days, and often earlier.
Patients who are newly diagnosed with cancer, or have just found out they have cancer again, qualify for this priority access. Our surgeons will make themselves available to see you right away, even for a second opinion. We want to help you start your treatment as soon as possible.
Let Us Help You Feel Whole Again
Whether you’re experiencing new symptoms or want a second opinion on a diagnosis, our dedicated digestive health experts are here to help you find answers and a path forward. Request an appointment today to take charge of your health and get the personal support you need.
