
Our Experience Helps Patients Live Better with Crohn’s Disease
The AdventHealth Digestive Health Institute has a special focus on caring for patients who have autoimmune, inflammatory bowel conditions such as Crohn’s disease. Crohn’s disease involves chronic inflammation that can be located anywhere in the gastrointestinal (GI) tract. The condition causes ulcers that can develop anywhere from the mouth to the anus, but are most commonly found in the small intestine. However, one of the ways Crohn’s disease differs from ulcerative colitis is that diseased areas can appear in multiple areas of the GI tract, with healthy tissue in between. Crohn’s does not necessarily affect only the colon as colitis does.
Besides causing bothersome symptoms, Crohn’s disease increases the chances a person will develop cancer in the GI tract. Crohn’s can also cause bowel blockage, which can be life-threatening. Because of the condition’s potential for severe complications, it is important to be treated by a team highly experienced in treating Crohn’s disease such as the one at AdventHealth Digestive Health Institute.
Striving to Treat Crohn’s in the Easiest Ways for Patients
Thanks to ongoing advances in medicine, more and more patients with Crohn’s disease will never need surgery. However, if surgical treatment becomes necessary, our patients benefit from the expertise of AdventHealth Digestive Health Institute's advanced colon and rectal surgeons. They can perform minimally invasive surgeries that lower the chance for complications and result in faster recoveries.
Crohn’s Disease Symptoms
Signs and symptoms of Crohn’s disease can include:
- Diarrhea that is severe and persistent
- Abdominal pain and cramping
- An abdominal mass that can be felt
- A tender abdomen
- Bloody stools
- Constipation
- Night sweats
- Skin problems
- Swollen joints
- An ulcer in the mouth or anus
Diagnosing Crohn’s Disease
Because Crohn’s disease symptoms can be a lot like ulcerative colitis or other gastrointestinal conditions, certain tests can help doctors make an accurate diagnosis. The exact mix of tests needed depends on the type and severity of a patient’s symptoms as well as his or her medical history.
Endoscopic, imaging and lab tests that can help doctors reach a Crohn’s diagnosis include:
- Colonoscopy with biopsy
- Flexible sigmoidoscopy
- Enteroscopy
- Capsule endoscopy
- CT scan or MRI
- Barium enema
- Stool tests
Crohn’s Disease Treatment – Medical Management
While a cure for Crohn’s disease does not yet exist, fortunately medicine for inflammatory bowel diseases has advanced considerably in recent years. Certain treatments help prevent flare ups and allow some patients with Crohn’s to experience significant periods of remission and avoid complications such as bowel obstruction.
The goal of medical treatment is to control the inflammation so that symptoms improve or even disappear. Medicines that can help decrease the body's inflammatory response include anti-inflammatory drugs and immunomodulators. These medicines can be given via IV or infusion, or taken orally. Sometimes antibiotics are prescribed, especially when patients have infections caused by Crohn’s disease. While the antibiotic’s purpose is to treat the infection, some patients find it also improves their other symptoms. Not every medicine used to manage Crohn’s disease works well for every patient. However, there are many different anti-inflammatory and immune suppressant drugs. Your doctor may need to adjust your medicines to find the right combination for you.
Surgery for Crohn’s Disease
Many patients with Crohn’s disease will eventually need surgical treatment. The most common reason Crohn’s patients need surgery is a bowel blockage. Other reasons for surgery include gastrointestinal bleeding, anal abscess, anal fistula or cancer.
Surgical procedures used to treat Crohn’s disease complications and symptoms include:
- Small bowel resection. When bowel obstruction occurs in the small intestine, some or most of the small intestine may be removed. The remaining bowel is usually reconnected. If this is not possible, then a permanent ileostomy will be created so that stool has a way to exit the body. At DHI, our colon and rectal surgeons strive to offer small bowel resection as a minimally invasive rather than an open procedure. This allows patients to have a shorter hospital stay and recover faster.
- Stricturoplasty. In certain cases, patients may be able to have an alternative to bowel resection called stricturoplasty. This procedure removes the scar tissue in the small intestine responsible for narrowing the intestine. It leaves the intestines connected, which means they work as usual after recovery. While stricturoplasty involves a long hospital recovery, it prevents short bowel syndrome which can lead to malnourishment.
- Colectomy. This surgery removes some or all of the colon. More details about colectomy can be found on the Colorectal Surgery page.
- Abdominoperineal resection. This surgery removes the anus, rectum, and sigmoid (lowest part of the) colon. It results in the need for a permanent external ostomy, so DHI surgeons will explore other options before considering this approach.
- Proctocolectomy. This surgery involves removing the rectum as well as some or all of the colon. Because the anus is left intact, a J-pouch surgery (described below) may be possible. J-pouch surgery allows patients to have normal bowel movements after they have fully recovered.
J-Pouch Surgery Helps Restore Normal Function for Patients.
Removing a part of the small intestine or colon results in a need for an ostomy, or new way for stool to exit the body. However, the colon and rectal surgeons at AdventHealth Digestive Health Institute are experienced in offering a way to do this that preserves normal function. The procedure is called an ileal pouch anal anastomosis, but it is better known as J-pouch surgery. The benefit of J-pouch surgery is that patients are not left with a permanent need for an abdominal opening and ostomy bag.
Inflammatory Bowel Disease
-
Crohn's Disease
Learn more about the symptoms, diagnosis and treatment of Crohn's disease
-
Ulcerative Colitis
AdventHealth Digestive Health Institute gastroenterologists and colorectal surgeons focus on treatment for colitis and irritable bowel syndrome.
-
Surgical Treatment for IBD
If medicine no longer works for treating Crohn’s disease or ulcerative colitis, surgery may be necessary.
-
Endoscopy Services for IBD
Our compassionate medical staff is committed to providing high-quality healthcare services in Hillsborough County.
-
Infusion Services
Sometimes medicine works better when it’s injected directly into the bloodstream, which is where infusion therapy comes in. Learn more about infusion services today.
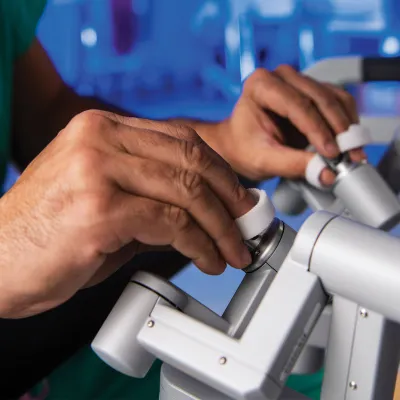
Recover Faster With Minimally Invasive and Robotic Surgery
All the surgeons at the AdventHealth Digestive Health Institute have a large depth of experience in offering minimally invasive surgery.

Meet Your Dedicated Experts
Our specialists are passionate about providing collaborative care that addresses your unique needs and goals while ensuring you feel informed and supported every step of the way. Learn more about our team and their areas of expertise.

Surgical Consultations For Digestive Cancer Without the Wait
Appointments Within Seven Days for Patients with Cancer
At AdventHealth Digestive Health Institute, we know that after being diagnosed with cancer, patients want and often need to begin treatment quickly. So we make it a priority to offer appointments for cancer surgery consultations within five business days, and often earlier.
Patients who are newly diagnosed with cancer, or have just found out they have cancer again, qualify for this priority access. Our surgeons will make themselves available to see you right away, even for a second opinion. We want to help you start your treatment as soon as possible.
