- AdventHealth Digestive Health Institute

As professional medical conferences have moved to virtual formats, this year many doctors have had new experiences. In early 2020, when he was invited to present at the 3rd Annual Association of Southeast Asian Nations (ASEAN) Laparoscopic Hepatopancreatobiliary (HPB) Surgery Conference, Iswanto Sucandy, MD, FACS, advanced HPB surgeon at the AdventHealth Digestive Institute Tampa, was expecting to travel to the Philippines in August. Instead, he was half a world away and at his computer at 2 am to speak to a group of international HPB surgeons. And, despite the late hour, he was pleased to do so.
“It is truly a great honor to be invited internationally to give this talk, especially by a professional group of surgeons in Asia,” says Dr. Sucandy. “The highest complexity and the finest minimally invasive liver, pancreas and biliary surgery is not typically done by surgeons in the West,” he adds, noting that Asian surgeons tend to be “the best HPB surgeons on earth.”
According to the conference organizers, the goal of the event was “to bring together current trends and innovations by giving talks that are idea-focused, and on a wide range [of] application and adaptation for a safe minimal access approach to HPB surgery.” In other words, nearly 1,000 attendees were present virtually to learn from and be inspired by the speakers, who presented on how to give patients better minimally invasive surgery outcomes.
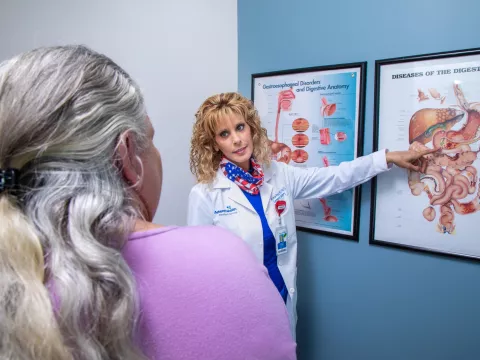
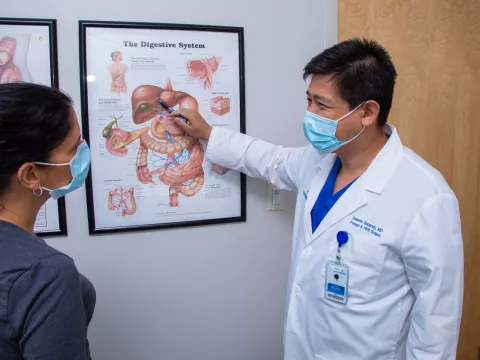
HPB surgery – that is, surgery for the liver (hepato), pancreas (pancreato) and/or bile ducts (biliary) – is often performed as an open operation. This involves a large, abdominal incision. However, Dr. Sucandy and his Digestive Institute (DI) colleagues, Alexander Rosemurgy, MD, FACS, and Sharona Ross, MD, FACS, both advanced foregut and HPB surgeons, are experienced in giving patients minimally invasive options. Minimally invasive surgery uses much smaller incisions and a camera that can see inside the body. Because this approach results in less trauma, patients recover from their operations faster with less pain and scarring. When it comes to operating on the liver and bile ducts, surgeons need extreme precision. Because of this, the DI surgeons very often use the da Vinci® Surgical System for their procedures. In fact, Dr. Sucandy was one of the earliest adopters of a robotic approach for liver surgery in the world.
Dr. Sucandy’s August 15 presentation at the ASEAN Laparoscopic HPB Conference and 2nd Philippine Association of Hepato-Pancreato-Biliary Surgeons (PABPBS) was entitled “Application of Robotic Technology in Major Minimally Invasive Liver Surgery. Added Value and Future Potentials.” He started off by mentioning that major liver surgery with the surgical robot is still very rare and limited to only certain high-volume centers that have much expertise in robotic liver surgery.
Robotic Liver Surgery in Tampa: A Safer and More Precise Approach
With minimally invasive major liver resection, the surgical robot gives the surgeon certain advantages over laparoscopy, an earlier minimally invasive surgical approach:
- A smaller chance the surgeon will have to change – or “convert” – to an open procedure. With laparoscopic hepatectomy (removal of a portion of the liver), surgeons often run into issues that cause them to abandon the minimally invasive approach. According to the medical literature, about 8 to 35 percent of laparoscopic liver operations are converted to open surgery. In the experience of the DI surgeons’ use of robotic liver surgery, this drops to about half a percent (about 1 in every 200 operations).
- A better view of the surgical site. Unlike laparoscopy, the surgical robot’s camera provides a magnified 3D view of the area being operated on. Also, the camera on the robot can be better controlled and kept still. This is very important during critical moments of the operation.
- A more minimally invasive approach. Even with laparoscopy, which uses thin sticks and catheters, the surgeon often has to place his or hand inside the patient’s body to complete liver procedures. However, this is unnecessary with robotic liver surgery. The surgical robot also allows surgeons to better manage any bleeding or bile leak that occurs during the operation and makes certain surgical steps in liver resection are easier and more precise. Ultimately, it gives patients a safer approach.
- An option for patients who have had prior liver procedures or other liver scarring. Some patients have had previous liver surgery or liver embolization procedures to treat their liver cancers. Other patients have cirrhosis. All of these scenarios cause scarring to the liver, making operations more difficult. However, the DI surgeons have found that even when scarring would make a laparoscopic approach nearly impossible, it is still feasible to use robotic liver surgery.
Results of Robotic Liver Surgery at Digestive Institute Tampa
Dr. Sucandy shared his, Dr. Rosemurgy and Dr. Ross’s results with the first 100 major robotic liver operations at DI – the largest series in America. These results were also published this year in a surgical journal article in the Annals of Surgical Oncology. Only once in 100 cases did the surgeons need to convert the robotic liver operation into an open procedure. Also, 99 percent of patients were alive 30 days after their robotic liver surgery at DI, and 98 percent 90 days after. Finally, patients who had robotic liver surgery typically only required 3 to 5 day hospital stays, depending on the portions of the liver they had removed. With traditional, open liver surgery, hospital stays are significantly longer.
Robotic Complex Liver and Bile Duct Surgery in Tampa
Dr. Sucandy spoke not just about major liver surgery but also about complicated cases that required him and his colleagues to rebuild the bile ducts in and around the liver. For example, Dr. Sucandy, Dr. Rosemurgy and Dr. Ross are using the surgical robot to offer minimally invasive treatment to patients with bile duct cancer. Removing the portions of the bile ducts with cancer tumors and reconstructing them so that bile can flow from the liver to the small intestine is a highly complex operation. Not many surgeons in the world offer a minimally invasive approach for this kind of complicated procedure. However, several times now the DI surgeons have successfully used the surgical robot to treat bile duct cancer (cholangiocarcinoma), including a specific type of bile duct cancer called Klatskin tumor.
If you might need surgery for a liver or bile duct cancer, trust the team experienced in offering minimally invasive, robotic operations. For an appointment with a DI advanced HPB surgeon, call
Call844-650-5950.