- AdventHealth Digestive Health Institute
Did you know that people who experience acid reflux might be at risk for esophageal cancer? This post explores the link between gastroesophageal reflux disease (GERD) and esophageal cancer, and why you might want to talk with a surgeon at the AdventHealth Digestive Institute Tampa if you’ve been diagnosed with GERD and have been on medications for it longer than a few weeks. By permanently treating GERD, some esophageal cancers can be prevented. However, if patients do develop cancer, the advanced foregut surgeons, Sharona Ross, MD, FACS, and Alexander Rosemurgy, MD, FACS, at the AdventHealth Digestive Institute Tampa offer minimally invasive surgical treatments for esophageal cancer that have been found to improve survival rates.
An Epidemic of Esophageal Cancer Caused by GERD
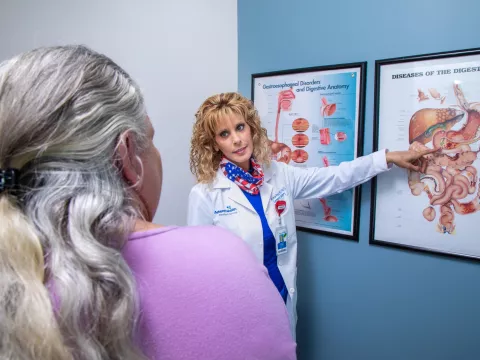
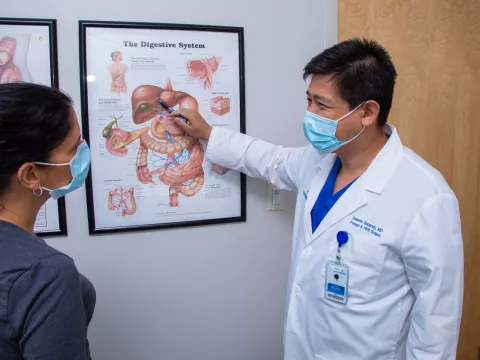
The esophagus is the tube that allows food to travel from the mouth to the stomach. Where the esophagus connects to the stomach is a valve called the lower esophageal sphincter, or LES. The LES allows food to move into the stomach and prevents stomach acid from flowing back up into the esophagus. However, as we age, a number of things – obesity, pregnancy, even weightlifting or chronic constipation – can cause pressure within the abdomen that creates a hiatal hernia that interferes with the LES. By age 60, more than half of adults have developed a hiatal hernia. Unfortunately, this means that the LES might not be able to close tightly enough, allowing stomach contents to flow back up into the esophagus.
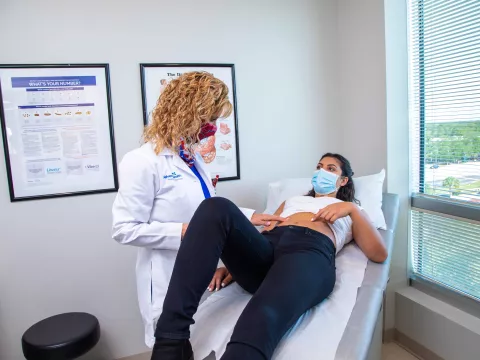
Many people experience this acid reflux phenomenon as heartburn, though it may also cause swallowing problems or a bad, bitter taste in the back of the mouth. It is normal for acid reflux to happen occasionally, but when people routinely experience it, they need to see their doctors. A gastroenterologist can run tests to determine whether a patient has chronic acid reflux. The gastroenterologists at the AdventHealth Digestive Institute Tampa have a number of tools – such as an upper endoscopy imaging study and the Bravo pH study that measures when and how much acid refluxes into the esophagus – to prove whether or not a patient has GERD.
Because of increased obesity rates, GERD has become more common in recent years. GERD is also why there has been a dramatic rise in esophageal cancer, particularly with a cancer called esophageal adenocarcinoma. From 1973 to 2010, the number of esophageal adenocarcinoma cases have increased 57 times! This cancer is caused when stomach acid and bile damage the bottom portion of the esophagus. Unlike the stomach lining, the esophagus cannot withstand these harsh substances the body uses to digest food. Having acid and bile in the esophagus can lead to irritation, then erosion, then ulcers, then abnormal cells and then Barrett’s esophagus – a condition in which cells that look like stomach cells are now in the lower part of the esophagus. Besides being painful, Barrett’s esophagus is a precancer, and patients who have it are about 50 times more likely to develop esophageal adenocarcinoma than those without the condition.
Why Long-Term Use of Acid-Blocking Medications Does Not Prevent Esophageal Cancer
You might think that patients with GERD can simply take medications such as “the purple pill” to find relief for their symptoms and reduce their risk for esophageal cancer. Unfortunately, while some drugs are very good at controlling GERD symptoms, they actually raise the risk for esophageal adenocarcinoma. Medications such as antacids, H2 blockers and proton pump inhibitors may neutralize or stop the stomach from producing acid, but they do not fix the problem of stomach contents refluxing into the esophagus. Even without acid, these reflux contents still contain bile, a base, that can cause cancer in the lining of the esophagus. In fact, because the acid that used to neutralize the bile is gone, the alkalinity of the stomach contents is raised, and they pose an even greater danger to the esophagus than before.
When the FDA approved the first proton pump inhibitor in 1989, patients were only expected to use them for six weeks out of the year. This medication was not intended to be used for months or years on end. During the past three decades when many patients have been using proton pump inhibitors chronically to control GERD, rates of esophageal adenocarcinoma have increased more than seven times over, at a steeper rate than previously. This is a very alarming statistic that deserves to be taken seriously. Instead of chronically using proton pump inhibitors or antacids, patients with GERD would be better served by having a minimally invasive procedure that cures the condition.
GERD Surgery: A Mechanical Solution to a Mechanical Problem
While long-term use of proton pump inhibitors can be dangerous for some patients, the good news is that there are minimally invasive surgical solutions that can permanently treat GERD. The Advanced Foregut and HPB Surgeons at AdventHealth Digestive Institute Tampa, Alexander Rosemurgy, MD, FACS, and Sharona Ross, MD, FACS, are both highly experienced in offering patients a procedure called fundoplication that tightens the closure of the LES valve between the esophagus and the stomach.
“GERD is a mechanical problem that requires a mechanical solution,” says Dr. Ross. “By using surgery to tighten the LES valve and repairing any hernia that is present, the valve can once again keep stomach contents out of the esophagus, and the patient is cured of GERD.”
Together, Dr. Ross and Dr. Rosemurgy have performed more than 3,500 of these fundoplication procedures. If a patient has never had a fundoplication before, the surgeons will likely offer them a laparo-endoscopic single site (LESS) procedure. Because this procedure involves only a 1.2 cm incision in the patient’s belly button, it is often called “scarless surgery”; the procedure is so minimally invasive that the patient will not look like he or she even had an operation. While this approach to fundoplication is not right for every patient, Dr. Ross and Dr. Rosemurgy can also offer other non-surgical solutions such as transoral incisionless fundoplication or the Stretta procedure to arrive at similar GERD treatment results.
After GERD surgery, a large majority of patients find that their symptoms are reduced enough that they can stop taking proton pump inhibitors or other medications that only mask their reflux issue while leaving them at risk for esophageal cancer. Many patients find complete relief from GERD after being treated by one of the AdventHealth Digestive Institute Tampa surgeons.
If you chronically take medication for GERD, you may be at high risk for esophageal cancer. Call 833-288-0248 for an appointment with Dr. Ross and Dr. Rosemurgy to discuss permanent treatment for GERD.