
AdventHealth Digestive Health Institute Offers Expert Treatment for Bile Duct Obstruction
Bile ducts, sometimes called the biliary tree or biliary system, allow bile to pass from the liver to the small intestine to help digest food. Unfortunately, bile ducts can become blocked. Gallstones or bile duct cancer (cholangiocarcinoma) are the usual causes of these blockages. However, injury to the bile ducts, often from prior gallbladder surgery, can result in bile duct obstruction as well. Rarer causes include abnormal bile duct narrowing, bile duct cysts or the enlargement of lymph nodes in the area.
The advanced gastroenterologists and Hepato-Pancreato-Biliary (HPB) surgeons at AdventHealth Digestive Health Institute have the necessary experience and skill to treat patients with bile duct obstruction.
Helping You Understand Bile Duct Obstruction
We know understanding your diagnosis can be confusing. But at the AdventHealth Digestive Health Institute, it’s our goal to make it easy for you to navigate your condition, understand your symptoms and know your treatment options.
When one of the bile ducts becomes blocked, patients often experience:
- Dark urine
- Fever
- Itching
- Jaundice, yellowing of the skin or eyes
- Loss of appetite
- Pain in the upper right side of the abdomen
- Stools that are clay-colored
If your doctor suspects you may have a bile duct blockage, tests will be done to determine the extent of the blockage and what is causing it.
In addition to a physical exam and lab test, you will likely need some of the following procedures:
- Imaging tests. Tests like ultrasounds, CT scans or MRIs reveal if a tumor is present and can provide very detailed images of the bile ducts and liver.
- Endoscopic retrograde cholangiopancreatography (ERCP). ERCP uses a lighted tube inserted through your mouth, down through the esophagus, into the stomach, into the small intestine (duodenum) and through the papilla of Vater to see the bile ducts.
- Cholangiogram. A cholangiogram is an X-ray of the bile ducts. Dye is injected, and X-rays are taken, which give a road map to the biliary tree. The test is performed along with an ERCP.
- Fine needle aspiration (FNA). If you have an area that could be a cancerous tumor, a biopsy of the tumor taken through an FNA may be done. An FNA involves a small needle that removes small samples of several layers of cells. This biopsy is usually done from the inside with an ERCP. A cholangiogram may also help the doctor know which areas to sample. The sampled cells get sent to a pathologist who can determine whether they are cancerous.
The goal of treatment is to physically remove the blockage. The method of doing this is determined by the cause and location of the obstruction.
For blockages at the sphincter of Oddi caused by gallstones. Stones can often be removed endoscopically during an ERCP procedure. This is a minimally invasive procedure that involves no external incisions. Part of the sphincter of Oddi, where the bile duct shared by the gallbladder and pancreas drains into the small intestine, is removed with small instruments on the end of the endoscope used for ERCP. This allows the stone causing the blockage to dislodge.
For blockages with other causes or in different locations. Surgery may be necessary.
Surgery is highly recommended if:
- A patient is getting sicker.
- The obstruction is getting worse.
- The blockage has caused a tear in the bile duct.
- A tumor mass (benign or malignant) is present. Completely removing the tumor is the only potential way to cure cancers of the lower bile duct.
- The ERCP used to dislodge the gallstone did not work, or the patient’s symptoms did not go away.
At the AdventHealth Digestive Health Institute, Dr. Sharona Ross strives to offer patients minimally invasive surgeries to correct bile duct obstruction. When these surgeries are performed laparoscopically instead of as open procedures, patients experience less pain after surgery and recover much faster.
Medical Minute: Bile Duct Disease With Dr. Sucandy
Bile duct disease is a blockage that prevents bile from traveling to the small intestine from the liver. Gallstones or bile duct cancer are the usual causes of these blockages. The good news is our advanced gastroenterologists and Hepato-Pancreato-Biliary (HPB) surgeons at the AdventHealth Digestive Health Institute have the expertise you need to treat your condition.
Iswanto Sucandy, MD, FACS, Foregut and Hepatopancreatic Biliary (HPB) surgeon at AdventHealth Tampa, discusses bile duct disease and a minimally invasive procedure for treating patients with this condition.
Pancreatic, Biliary and Gallbladder Disease
-
Bile Duct Diseases and Conditions
AdventHealth Digestive Health Institute gastroenterologists and gastrointestinal surgeons treat bile duct obstruction (blocked bile duct) and cholangiocarcinoma (bile duct cancer).
-
Endoscopy for Pancreatic, Bile Duct and Gallbladder Conditions
Gastroenterologists at AdventHealth Digestive Health Institute use ERCP and endoscopic ultrasound to diagnose and treat pancreas, gallbladder and bile duct diseases.
-
Gallbladder Cancer
Removing the gallbladder with cancer is a very complex surgery that requires highly experienced surgeons like those at AdventHealth Digestive Health Institute.
-
Gallbladder Conditions
Advanced surgeons at AdventHealth Digestive Health Institute provide cholecystectomy and other treatments for gallbladder pain and gallstones.
-
Gallbladder Surgery
Surgeons at the AdventHealth Digestive Health Institute provide advanced, scar-less cholecystectomy for gallbladder pain and gallstones.
-
Pancreatic Cancer
Our surgeons are among the region’s most experienced in pancreatic surgery. We can help treat your cancer with minimally invasive options. Learn more today.
-
Pancreatic Conditions
Gastroenterologists and surgeons at AdventHealth Digestive Health Institute are experts for treating Pancreatitis, Pancreatic Cyst and other conditions of the pancreas.
-
Pancreatic Surgery
AdventHealth Digestive Health Institute's pancreas surgeons offer minimally invasive pancreatectomy for Pancreatitis, Pancreatic Cysts and Pancreatic Cancer. Learn more.
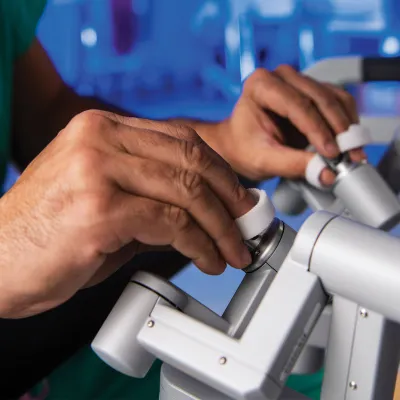
Recover Faster With Minimally Invasive and Robotic Surgery
The expert surgeons at the AdventHealth Digestive Health Institute have a large depth of experience in offering minimally invasive surgery.

Meet Your Dedicated Experts
Our specialists are passionate about providing collaborative care that addresses your unique needs and goals while ensuring you feel informed and supported every step of the way. Learn more about our team and their areas of expertise.

Surgical Consultations For Digestive Cancer Without the Wait
Appointments Within Seven Days for Patients with Cancer
At AdventHealth Digestive Health Institute, we know that after being diagnosed with cancer, patients want and often need to begin treatment quickly. So we make it a priority to offer appointments for cancer surgery consultations within five business days, and often earlier.
Patients who are newly diagnosed with cancer, or have just found out they have cancer again, qualify for this priority access. Our surgeons will make themselves available to see you right away, even for a second opinion. We want to help you start your treatment as soon as possible.
Let Us Help You Feel Whole Again
Whether you’re experiencing new symptoms or want a second opinion on a diagnosis, our dedicated digestive health experts are here to help you find answers and a path forward. Request an appointment today to take charge of your health and get the personal support you need.

